Heart Failure: What It Is and How to Manage It
Did you know that about 6 million adults in the U.S. live with heart failure? It’s not just an old‑person problem – anyone with high blood pressure, a history of heart attacks, or certain genetic conditions can develop it. In plain terms, heart failure means your heart isn’t pumping blood as efficiently as it should. That doesn’t always mean a “weak” heart; sometimes the heart is stiff, or it’s overloaded with fluid. Understanding the basics helps you spot trouble early and take control.
Key Symptoms You Shouldn't Ignore
The first sign most people notice is shortness of breath – especially when climbing stairs or lying flat at night. That feeling of not getting enough air is your body’s way of saying the heart can’t keep up with oxygen demand. Next, look for swelling in the ankles, feet, or even the abdomen; fluid builds up because blood backs up in the veins.
Fatigue is another big clue. If you’re constantly wiped out after a short walk, your heart may be struggling to deliver enough energy‑rich blood. Rapid weight gain over a few days (often just 2–3 lb) can signal fluid retention and needs immediate attention. Finally, persistent coughing or wheezing, especially at night, often points to fluid in the lungs.
Treatment Options That Actually Work
Good news: heart failure is manageable with a mix of medication, lifestyle tweaks, and sometimes devices. ACE inhibitors (like lisinopril) and ARBs help relax blood vessels, lowering the pressure your heart has to pump against. Beta‑blockers (such as carvedilol) slow the heartbeat just enough to give the heart a chance to recover.
Diuretics are the go‑to for fluid buildup – think of them as a gentle “water pill” that helps you shed excess pounds and eases swelling. Newer drugs called ARNIs (sacubitril/valsartan) combine benefits of both ACE inhibitors and ARBs, offering extra protection for many patients.
Beyond pills, lifestyle changes make a huge difference. Cut sodium to less than 2 g per day – that’s about a teaspoon of salt – to keep fluid from seeping into your tissues. Aim for at least 150 minutes of moderate activity each week; even short walks can boost circulation and stamina.
Weight management matters, too. Even a modest loss of 5–10 % of body weight can lower the heart’s workload dramatically. Keep track of daily fluid intake (usually around 1.5‑2 L) and talk to your doctor about any needed restrictions.
If medication isn’t enough, doctors might recommend devices. An implantable cardioverter‑defibrillator (ICD) protects against dangerous rhythms, while a left ventricular assist device (LVAD) can take over part of the pumping job in severe cases.
Finally, regular check‑ups are key. Blood tests, echo scans, and symptom logs help your healthcare team adjust treatment before problems get worse. Don’t wait for a crisis – schedule that follow‑up and bring a list of any new symptoms.
Heart failure can feel overwhelming, but with the right plan it’s something you can live with and even improve. Stay alert to symptoms, stick to your medication routine, watch what you eat, stay active, and keep an open line with your doctor. Your heart may need help, but you’ve got plenty of tools to give it a fighting chance.
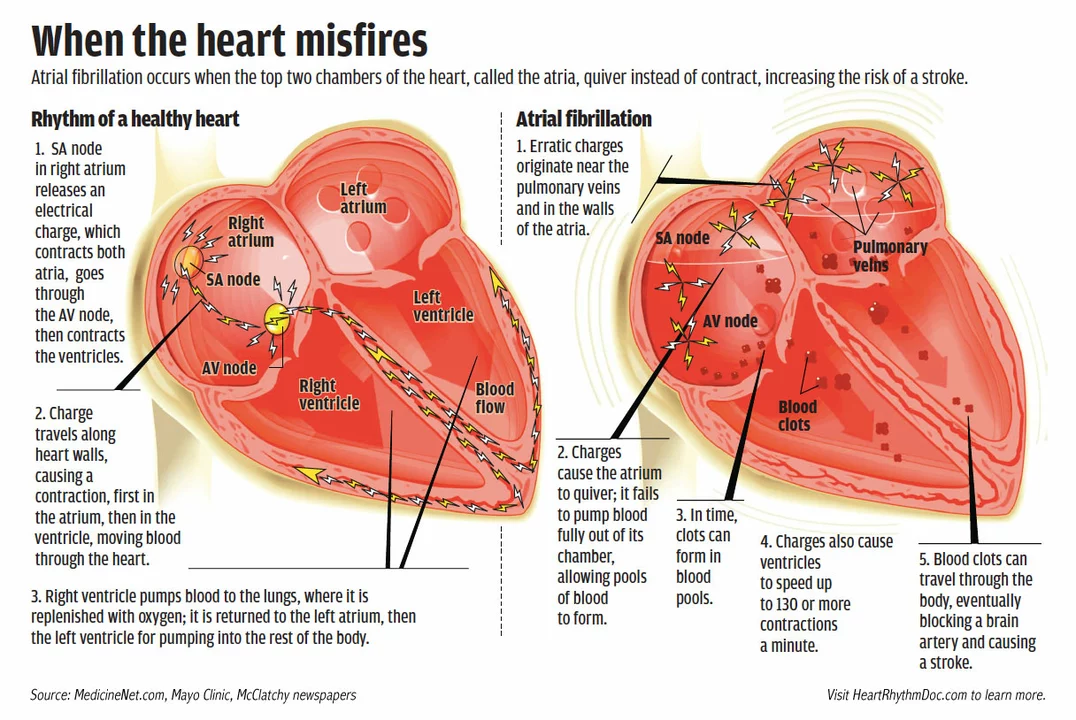
Atrial Fibrillation and Heart Failure: A Dangerous Duo
- 6