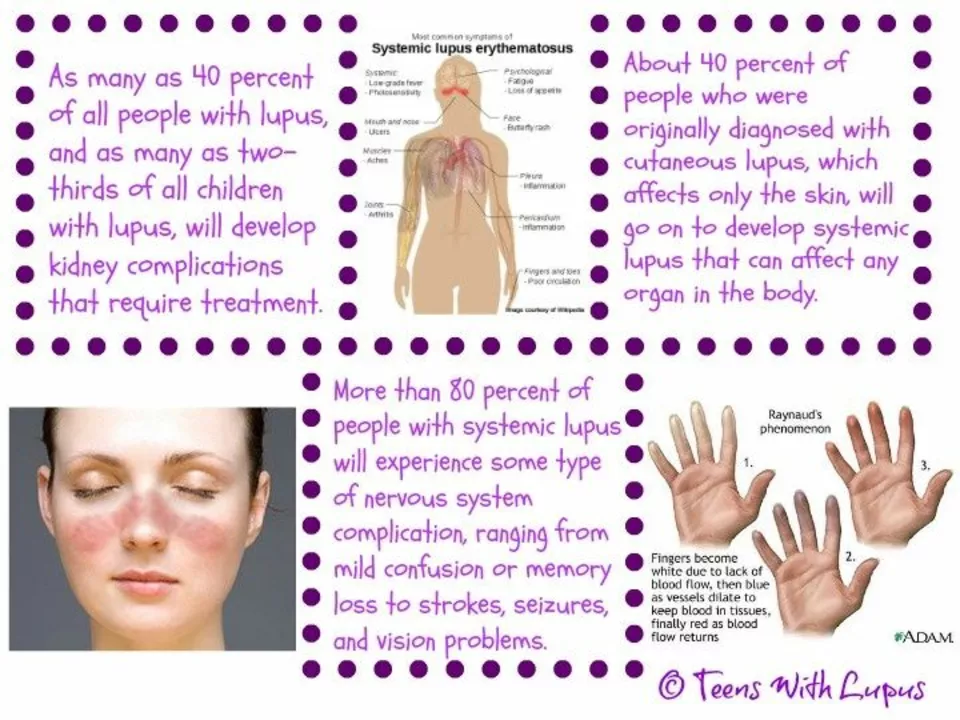
Systemic Lupus Erythematosus (SLE) – What You Need to Know
If you or someone you love has been told they have systemic lupus erythematosus, also called SLE or just lupus, the first reaction is often "what now?". It’s a chronic autoimmune disease that can affect skin, joints, kidneys, heart and many other parts of the body. The good news is that with early diagnosis, proper meds, and everyday habits, most people keep a fairly normal life.
Spotting the Common Signs
Lupus doesn’t show up the same way for everyone, but there are a few red flags to watch. The classic butterfly rash across the cheeks and nose pops up in many cases, as does joint pain that feels like arthritis but without major swelling. Fatigue is another big one – you might feel wiped out even after a full night’s sleep. Fever, hair loss, and sensitivity to sunlight also pop up fairly often. If any of these symptoms linger for weeks or keep coming back, it’s worth getting blood tests (ANA, anti‑dsDNA) that can confirm SLE.
How Doctors Treat Lupus
The backbone of lupus treatment is medication that calms the immune system. Hydroxychloroquine is the go‑to drug for many because it helps skin rashes and joint pain while being relatively safe for long‑term use. If you have more severe organ involvement, doctors might add steroids like prednisone for quick control, then taper down to steroid‑sparing options such as methotrexate or mycophenolate. Newer biologics, like belimumab, target specific immune pathways and are useful when other meds don’t work.
Besides pills, regular check‑ups are key. Blood work every few months tracks kidney function, blood counts and inflammation levels. If you’re on steroids, keep an eye on bone health – calcium, vitamin D, and sometimes a bisphosphonate can prevent loss.
Living with Lupus Day‑to‑Day
Medication is only half the battle. Simple lifestyle tweaks make a big difference. Sun protection isn’t just for beach days; wear a broad‑spectrum SPF 30+ daily, even when it’s cloudy. A balanced diet rich in omega‑3 fats (think salmon, walnuts) can ease inflammation. Gentle exercise – walking, swimming, yoga – improves joint flexibility and lifts mood without overloading joints.
Stress management matters too. Many people notice flare‑ups after a stressful week. Try short meditation sessions, breathing exercises, or hobbies that relax you. And don’t skip sleep – aim for 7–9 hours each night to keep the immune system in check.
If you’re feeling overwhelmed, remember you’re not alone. Support groups, whether online or local, let you share experiences and tips with folks who truly get it. Your doctor can also refer you to a rheumatologist who specializes in lupus care.
Bottom line: systemic lupus erythematosus is a complex condition, but with the right meds, regular monitoring, and everyday self‑care, most people stay active and enjoy life. Keep asking questions, stick to your treatment plan, and lean on community resources – they’ll help you manage SLE more confidently.