Insulin Resistance Explained: What It Is and How to Beat It
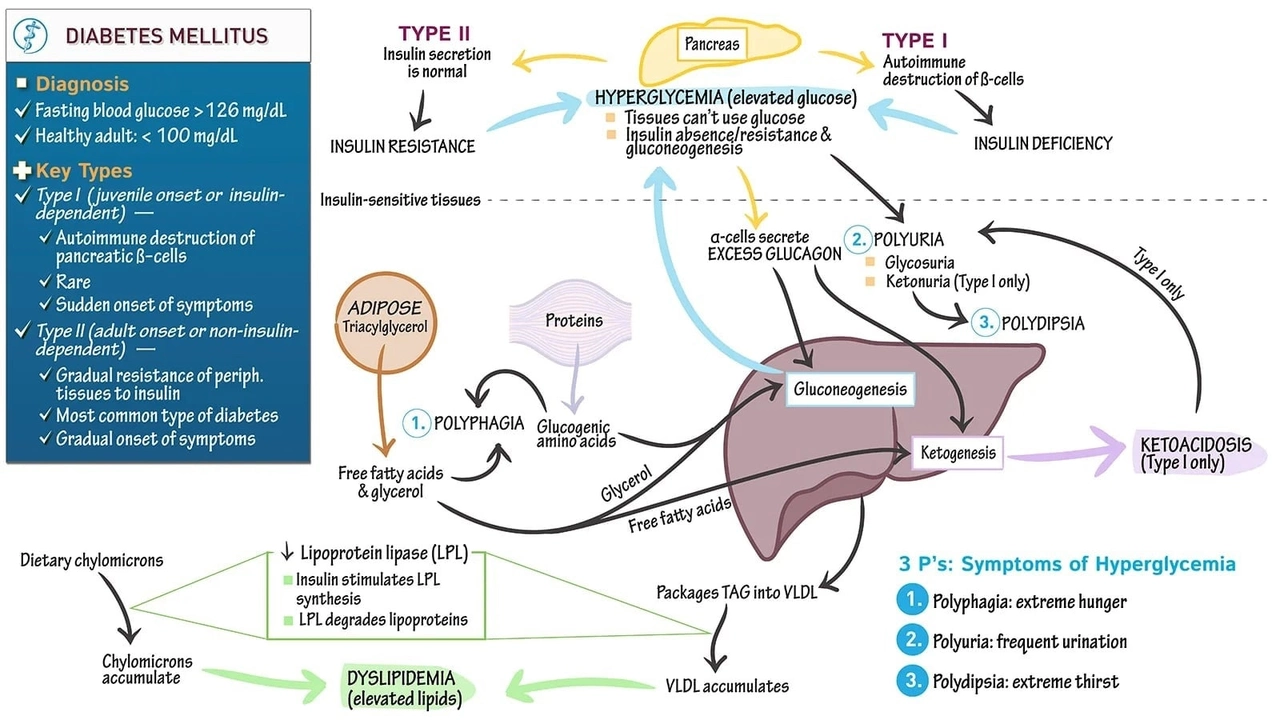
If your doctor mentioned "insulin resistance" and you walked away confused, you’re not alone. In plain terms, it means your body’s cells aren’t listening to insulin the way they should. Insulin is the hormone that tells sugar (glucose) to move from your blood into cells for energy. When cells ignore the signal, blood sugar stays high and the pancreas works overtime, eventually wearing out.
Why Insulin Resistance Happens
The main culprits are excess calories, especially from refined carbs and sugary drinks, plus too much belly fat. Fat around your abdomen releases inflammatory chemicals that mess with insulin’s signaling pathway. Genetics play a role, but lifestyle choices often tip the scale. Even a sedentary job can push you toward resistance because muscles need activity to pull glucose from the bloodstream.
Easy Lifestyle Tweaks That Lower Resistance
First, move more. You don’t need marathon training; 30 minutes of brisk walking, cycling, or even dancing a few times a week can boost insulin sensitivity dramatically. Next, watch your carbs. Swap white bread and pastries for whole grains, legumes, and veggies. The fiber in these foods slows glucose absorption, keeping spikes low.
Second, add protein to every meal. Protein blunts the rise in blood sugar after eating and helps preserve lean muscle mass—the tissue that actually uses insulin. A handful of nuts, a boiled egg, or some Greek yogurt are simple options.
Third, prioritize sleep. Less than 6‑7 hours a night raises cortisol, a stress hormone that directly interferes with insulin’s work. Aim for consistent bedtime routines and keep the room dark and cool.
Finally, manage stress. Chronic stress keeps your body in “fight or flight” mode, flooding it with hormones that raise blood sugar. Activities like deep breathing, short walks, or a hobby you love can lower those levels fast.
What to Eat (and What to Skip)
Focus on foods rich in magnesium and omega‑3s—think leafy greens, avocado, salmon, and chia seeds. These nutrients improve cell membrane function, making it easier for insulin to do its job. On the flip side, cut back on sugary sodas, candy, processed snacks, and anything labeled "low‑fat" but loaded with sugar.
Even a small change, like replacing your afternoon soda with sparkling water infused with lemon, can shave off unnecessary carbs. Over time those tiny swaps add up to big gains in insulin sensitivity.
Tracking Progress Without the Lab
You don’t need constant blood tests to see if you’re improving. Notice how often you feel hungry, your energy levels after meals, or whether you’re gaining weight around the waist. A steady drop in those signs usually means insulin is working better.
If you can, grab a cheap at‑home glucose meter and test first thing in the morning for a week. A consistent reading under 100 mg/dL signals good control; higher numbers suggest you still have work to do.
Bottom line: insulin resistance is reversible for most people with the right habits. Start small—move a bit more, swap one sugary drink, and get enough sleep. Those steps will put your cells back on speaking terms with insulin, keeping blood sugar steady and health on track.