Atrial Fibrillation: What It Is and How to Manage It
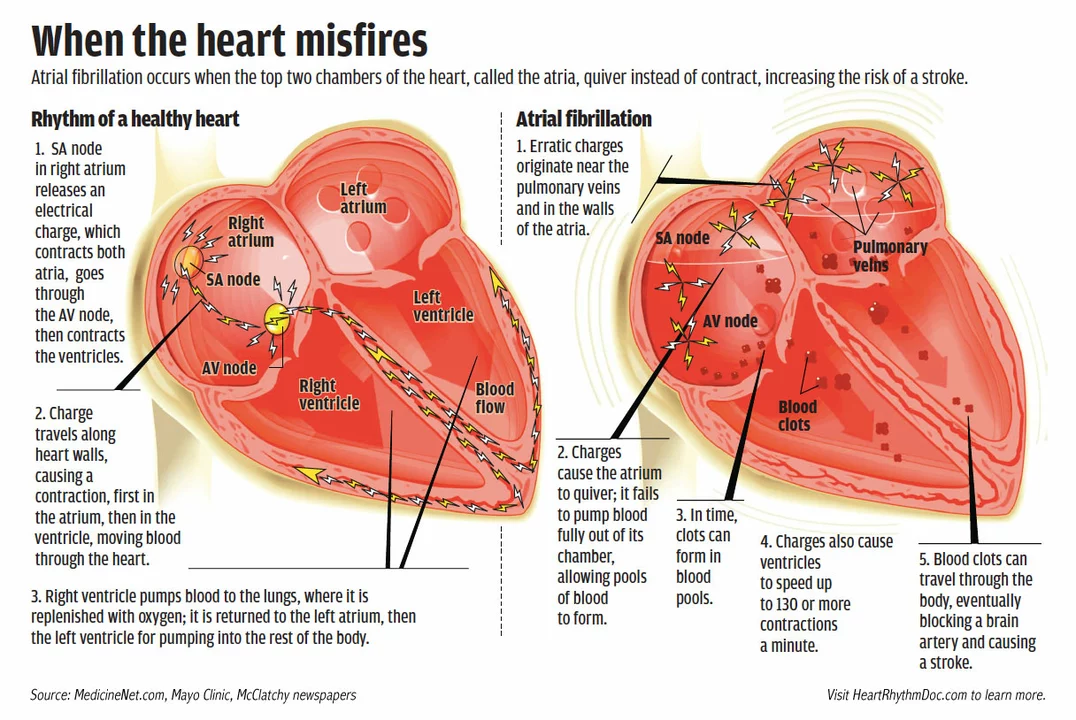
You've probably heard the term "atrial fibrillation" (or AFib) tossed around, but what does it really mean? In simple words, it's a heart rhythm problem where the upper chambers (atria) beat fast and irregularly. This chaotic beating can make your heart feel like it’s racing or skipping beats.
Most people notice a fluttering sensation in their chest, shortness of breath, or an unusual fatigue that doesn't go away with rest. Some folks hear a rapid heartbeat when they check their pulse. If you experience any of these signs, especially if they're new, it's worth getting checked by a doctor.
Understanding Atrial Fibrillation
AFib isn’t just an annoying irregular beat – it can raise the risk of blood clots, stroke, and even heart failure. The erratic motion prevents blood from flowing smoothly, which lets clots form in the atria. Those clots can travel to the brain and cause a stroke.
There are three main types: occasional (paroxysmal), persistent, and permanent. Paroxysmal AFib comes and goes on its own, while persistent stays longer and often needs medical intervention. Permanent AFib means doctors have decided not to try restoring a normal rhythm.
Common Treatments & Medications
The first goal is to control the heart rate so you don’t feel dizzy or short‑of‑breath. Doctors often prescribe beta‑blockers like Inderal (propranolol) or newer options such as metoprolol. These drugs slow down the heartbeat without fixing the irregular pattern, but they make life more comfortable.
If rhythm control is needed—meaning you want the heart to beat regularly again—anti‑arrhythmic pills like amiodarone may be used, or procedures like electrical cardioversion can reset the rhythm. Your doctor will decide based on age, overall health and how long AFib has been present.
Because clots are a big worry, most people with AFib take anticoagulants. Warfarin was the classic choice, but newer direct oral anticoagulants (DOACs) such as apixaban or rivaroxaban are easier to manage and need less monitoring.
Lifestyle tweaks also help. Cutting back on caffeine, alcohol, and smoking can reduce episodes. Regular exercise—just moderate activities like walking—keeps the heart healthier without over‑exertion.
Stay in touch with your healthcare team. They might order an ECG or wearable monitor to track how often AFib shows up. Adjusting meds based on those readings keeps you safe and reduces emergency visits.
Bottom line: atrial fibrillation is manageable when you know the signs, take prescribed medicines like beta‑blockers or anticoagulants, and adopt heart‑friendly habits. If something feels off, don’t wait—talk to a professional and get your rhythm back under control.
Atrial Fibrillation and Heart Failure: A Dangerous Duo
- 6